What is Steroid (Cortisone)?
Cortisone is naturally produced in the body through the adrenal gland and released when the body is under stress. Injectable cortisone is synthetically produced and is similar to the body’s own version. It works by minimising inflammation; this, in turn, will reduce your pain. ‘Cortisone’ injections have been used by orthopaedic professionals since the early 1950’s for a variety of conditions, including tendonitis, arthritis, tennis elbow, Morton’s neuroma, plantar fasciitis and carpal tunnel syndrome. It is completely legal and different from the illegal anabolic steroids used by some athletes.
Cortisone is not a pain-relieving medication, but rather works by minimizing the body’s reaction to inflammation. When the inflammation is lessened, the pain is as well. By injecting the steroid directly into the inflamed area such as a knee or shoulder joint, high concentrations of cortisone can be administered with minimal side effects. Discomfort usually improves within a few days and the benefits may be temporary, or permanent. If cortisone injections are used, they must be combined with appropriate rest periods and rehabilitation to gain the best results. Cortisone can take up to 3-4 weeks to be completely effective.
There are very few contraindications to the use of cortisone injections, however, in this clinic we do not inject patients with any of the conditions below:-
- Joint infection
- Skin infection at the site of the injection
- Previous allergic reaction to cortisone injections
- Joints with prosthesis – total knee/hip/shoulder replacements
- Pregnant patients
- Patients on antibiotics, unless long term or patients who have had a flu jab within the last 2 weeks
Precautions: Patients on blood thinning drugs – warfarin/heparin can have a cortisone injection if their INR is stable.
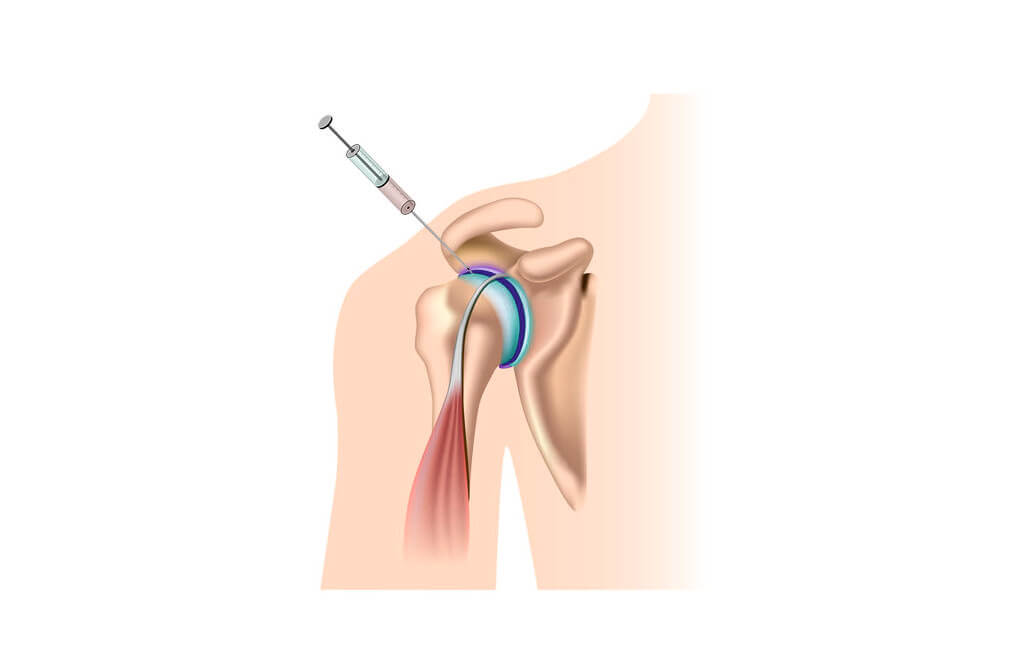
After the skin surface is thoroughly cleaned, the joint is entered with a needle attached to a syringe and injected into the joint space. Joint injections are given to treat inflammatory joint conditions, such as rheumatoid arthritis, psoriatic arthritis and osteoarthritis. This technique also applies to injections into a bursa or tendon to treat tendonitis and bursitis. Commonly injected joints include the knee, shoulder, ankle, elbow and small joints of the hand and feet.
As with nearly any procedure where medications are injected into the body, adverse reactions may occur.
- There may be bruising, bleeding or allergic reactions to the medicine injected into the joint.
- Post injection ‘flare’ has been reported in about 2% of patients. This occurs when the injected cortisone crystallises and causes pain worse than before the injection. Fortunately these ‘flares’ usually do not last long and resolve with ice and appropriate pain killers after 12 to 48 hours.
- Whitening of the skin around the injection site is also a common side effect, especially in darker skinned individuals. This discoloration is not harmful and is usually reversible.
- Diabetic patients may experience a temporary but significant elevation in their blood sugars due to absorption of the cortisone into the blood stream. We ask that you monitor your blood sugars for between 24 and 48 hours post injection, if appropriate.
- Infection at the injection site is a rare side effect. This can be avoided with proper skin sterilisation and by avoiding injecting individuals who show signs of infection in their body or who are on antibiotics for an acute infection, or who have had a live vaccine (flu, TB) injected into their system in the 2 weeks prior to the injection date.
If you have any further queries about receiving a cortisone (steroid) injection please do not hesitate to ask your injecting clinician, who would be happy to go over your concerns with you.
