I was told I have a hip bursitis. Do I need a hip replacement?
Overview
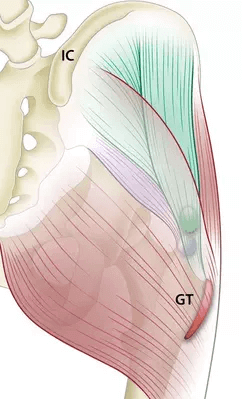
One of the most common dysfunctions of the hip joint is described by hip pain on the outside hip bone, especially sore during the night if lying on it or after long periods of standing/walking, where, despite the fact that there may be some underlying arthritis, this is usually not it’s cause. As said above, it tends to be a dysfunction, rather than an injury or damage to some structures in the hip area.
What is Trochanteric Bursitis?
Most people will hear clinicians call it a “Trochanteric Bursitis”, which describes an inflammation of the “Trochanteric Bursa”. The Trochanteric Bursa is a slim sack of fluid that is located just over the outside hip bone (Greater Trochanter) and in between the muscle group on the outside of your hip (Gluteus Muscle Group) and it’s main function is to provide padding to the bony prominence and to prevent significant amount of friction of the muscles and other tissues that overlap that bony prominence. (Figure 1)
How is Bursitis of the Hip diagnosed?
Your Physio will also be able to assess the contribution of any past or silent dysfunction of the spine or knee and ankle joints that may be contributing to the lack of improvement of your hip condition, as well us understand if your symptoms are actually referred from a spinal problem, rather than being a hip problem.
Request An Appointment with Lakky Physio
What is the treatment for Hip Bursitis?
The treatment for this condition usually consists of rest from aggravating activities, cold therapy on the area of pain and, then, gradual return to normal activities of daily living. On more painful cases, some doctors will consider a Steroid Injection into the bursa in order to reduce the inflammation, but this may still not resolve the most stubborn cases.
Greater Trochanteric Pain Syndrome(GTPS)
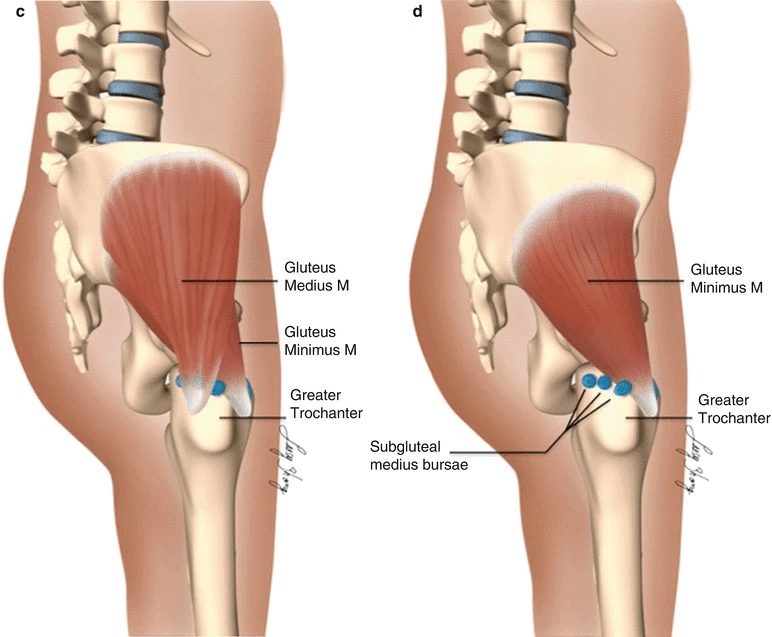
More recently, researchers found that this condition is often more than a simple bursa irritation and that it is associated with a tendinopathy of some hip muscles (the gluteus medius and minimus) and agreed to start calling it Greater Trochanteric Pain Syndrome(GTPS). This may explain why sometimes the passive approach of a Corticosteroid Injection may not be enough. Tendons are part of the system that moves our body, therefore they will need to be rehabilitated through exercises and gradual progression of load (Figure 2).
As we discussed on a previous article on Sciatica, leg pain can be caused by active trigger points on these gluteus hip muscles, therefore Greater Trochanteric Pain Syndrome(GTPS) can give you leg pain and be an alternative cause for what you think is a Sciatica presentation.
For more stubborn cases, which failed to resolve significantly with the above, apart from these treatments, NICE guidelines also suggest the use of Shockwave Therapy (Figure 3) as a last resort approach.
Some research also suggests that complementing all the treatments above with Acupuncture and Dry Needling may also be of benefit.
Fortunately, you can have all of the above-mentioned treatments with our team at Lakky Physiotherapy, so there is no need to be in pain.
References:
- Peng P.W.H. (2015) Hip: Intra-articular and Trochanteric Bursitis Injections. In: Regional Nerve Blocks in Anesthesia and Pain Therapy. Springer, Cham
- Chowdhury R, Naaseri S, Lee J, Rajeswaran G., (2014), Imaging and management of greater trochanteric pain syndrome. Postgrad Med J., Oct: 90(1068):576-81. doi: 10.1136/postgradmedj-2013-131828. Epub 2014 Sep
- Reid D. (2016) The management of greater trochanteric pain syndrome: a systematic review. Journal of Orthopaedics 13 (1), 15,28
- 2011, Extracorporeal shockwave therapy for refractory greater trochanteric pain syndrome. Interventional procedures guidance [IPG376]. UK: NICE guidelines. Available at: https://www.nice.org.uk/guidance/ipg376/chapter/1-Guidance
- EMS-dolorcast, 2019, Greater Trochanteric Pain Syndrome. [ONLINE] Available at: https://www.ems-dolorclast.com/en/greater-trochanteric-pain-syndrome [accessed 30 January 2019]
